Search
- Page Path
- HOME > Search
- Diabetes, obesity and metabolism
Big Data Articles (National Health Insurance Service Database) - Risk of Cause-Specific Mortality across Glucose Spectrum in Elderly People: A Nationwide Population-Based Cohort Study
- Joonyub Lee, Hun-Sung Kim, Kee-Ho Song, Soon Jib Yoo, Kyungdo Han, Seung-Hwan Lee, Committee of Big Data, Korean Endocrine Society
- Endocrinol Metab. 2023;38(5):525-537. Published online September 7, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1765

- 1,597 View
- 91 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
This study investigated the risk of cause-specific mortality according to glucose tolerance status in elderly South Koreans.
Methods
A total of 1,292,264 individuals aged ≥65 years who received health examinations in 2009 were identified from the National Health Information Database. Participants were classified as normal glucose tolerance, impaired fasting glucose, newly-diagnosed diabetes, early diabetes (oral hypoglycemic agents ≤2), or advanced diabetes (oral hypoglycemic agents ≥3 or insulin). The risk of system-specific and disease-specific deaths was estimated using multivariate Cox proportional hazards analysis.
Results
During a median follow-up of 8.41 years, 257,356 deaths were recorded. Diabetes was associated with significantly higher risk of all-cause mortality (hazard ratio [HR], 1.58; 95% confidence interval [CI], 1.57 to 1.60); death due to circulatory (HR, 1.49; 95% CI, 1.46 to 1.52), respiratory (HR, 1.51; 95% CI, 1.47 to 1.55), and genitourinary systems (HR, 2.22; 95% CI, 2.10 to 2.35); and neoplasms (HR, 1.30; 95% CI, 1.28 to 1.32). Diabetes was also associated with a significantly higher risk of death due to ischemic heart disease (HR, 1.70; 95% CI, 1.63 to 1.76), cerebrovascular disease (HR, 1.46; 95% CI, 1.41 to 1.50), pneumonia (HR, 1.69; 95% CI, 1.63 to 1.76), and acute or chronic kidney disease (HR, 2.23; 95% CI, 2.09 to 2.38). There was a stepwise increase in the risk of death across the glucose spectrum (P for trend <0.0001). Stroke, heart failure, or chronic kidney disease increased the risk of all-cause mortality at every stage of glucose intolerance.
Conclusion
A dose-dependent association between the risk of mortality from various causes and severity of glucose tolerance was noted in the elderly population. -
Citations
Citations to this article as recorded by- The Characteristics and Risk of Mortality in the Elderly Korean Population
Sunghwan Suh
Endocrinology and Metabolism.2023; 38(5): 522. CrossRef
- The Characteristics and Risk of Mortality in the Elderly Korean Population

- Diabetes, obesity and metabolism
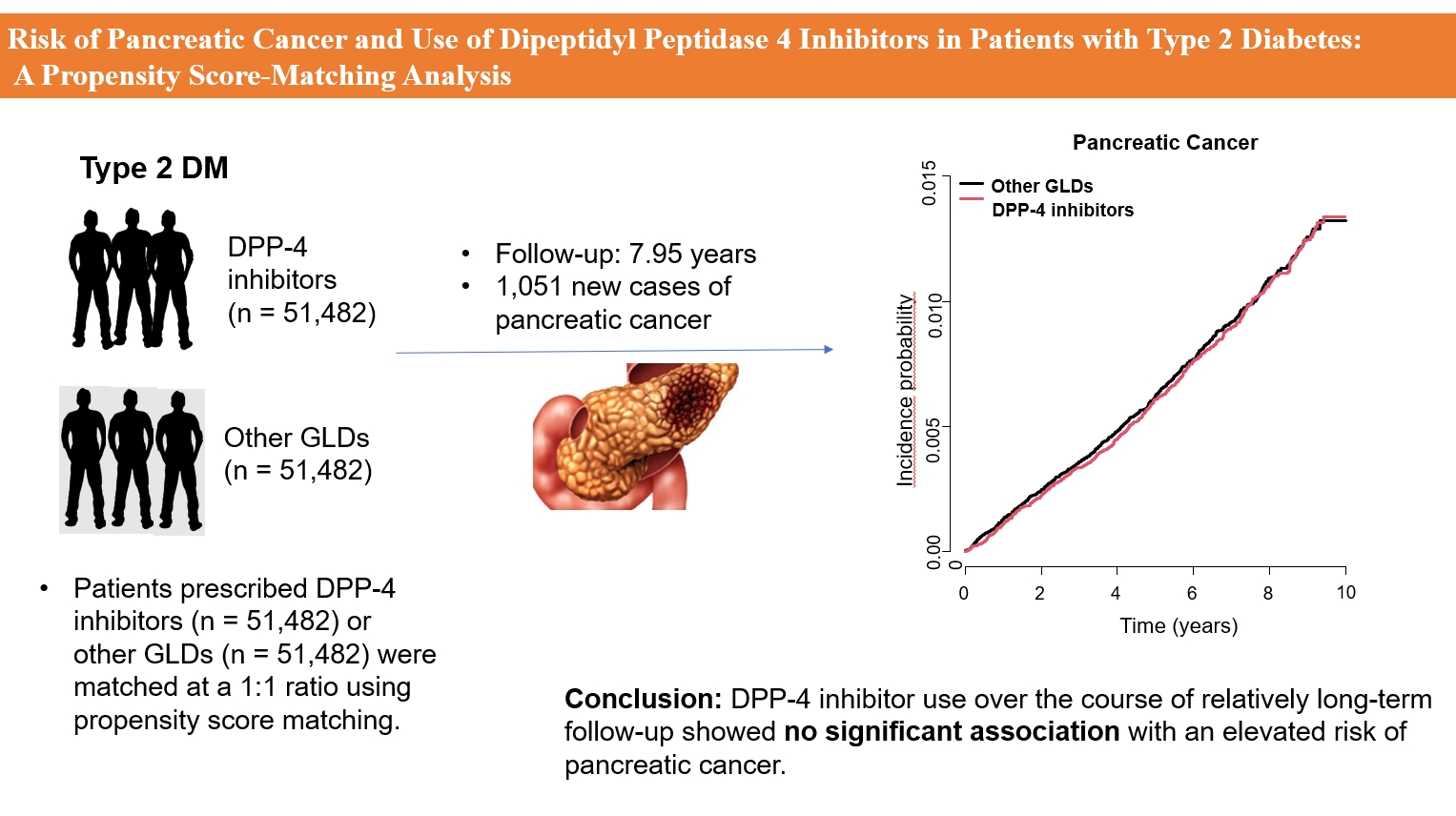
- Risk of Pancreatic Cancer and Use of Dipeptidyl Peptidase 4 Inhibitors in Patients with Type 2 Diabetes: A Propensity Score-Matching Analysis
- Mee Kyoung Kim, Kyungdo Han, Hyuk-Sang Kwon, Soon Jib Yoo
- Endocrinol Metab. 2023;38(4):426-435. Published online July 20, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1737
- 2,120 View
- 135 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
The effects of dipeptidyl peptidase 4 (DPP-4) inhibitors over the course of long-term treatment remain unclear, and concerns have been raised regarding the role of DPP-4 inhibitors in carcinogenesis in the pancreas. Earlier studies of pancreatic adverse events have reported conflicting results.
Methods
This study analyzed Korean National Health Insurance Service data from January 2009 to December 2012. Patients who had type 2 diabetes mellitus and took two or more oral glucose-lowering drugs (GLDs) were included. Patients prescribed DPP-4 inhibitors (n=51,482) or other GLDs (n=51,482) were matched at a 1:1 ratio using propensity score matching. The risk of pancreatic cancer was calculated using Kaplan-Meier curves and Cox proportional-hazards regression analysis.
Results
During a median follow-up period of 7.95 years, 1,051 new cases of pancreatic cancer were identified. The adjusted hazard ratio (HR) for DPP-4 inhibitor use was 0.99 (95% confidence interval [CI], 0.88 to 1.12) compared with the other GLD group. In an analysis limited to cases diagnosed with pancreatic cancer during hospitalization, the adjusted HR for the use of DPP-4 inhibitors was 1.00 (95% CI, 0.86 to 1.17) compared with patients who took other GLDs. Using the other GLD group as the reference group, no trend was observed for elevated pancreatic cancer risk with increased DPP-4 inhibitor exposure.
Conclusion
In this population-based cohort study, DPP-4 inhibitor use over the course of relatively long-term follow-up showed no significant association with an elevated risk of pancreatic cancer. -
Citations
Citations to this article as recorded by- Diabetes Duration, Cholesterol Levels, and Risk of Cardiovascular Diseases in Individuals With Type 2 Diabetes
Mee Kyoung Kim, Kyu Na Lee, Kyungdo Han, Seung-Hwan Lee
The Journal of Clinical Endocrinology & Metabolism.2024;[Epub] CrossRef
- Diabetes Duration, Cholesterol Levels, and Risk of Cardiovascular Diseases in Individuals With Type 2 Diabetes

- Diabetes, obesity and metabolism
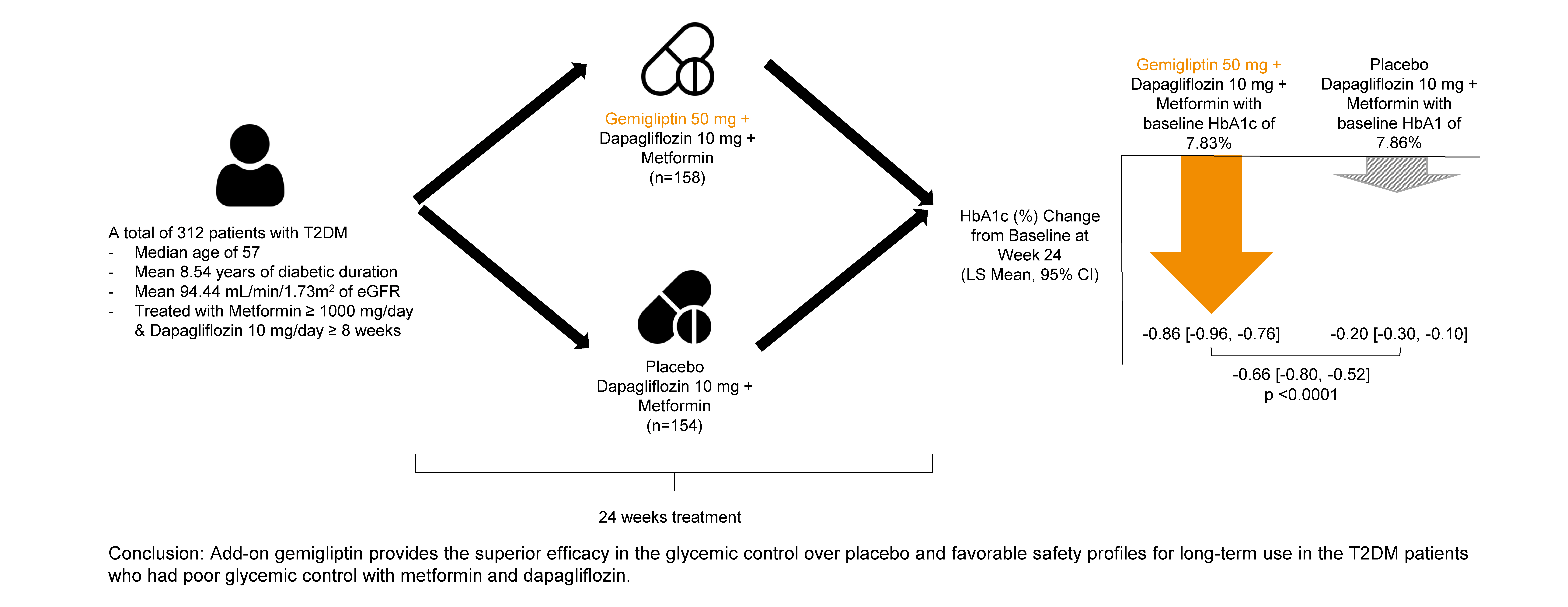
- Efficacy of Gemigliptin Add-on to Dapagliflozin and Metformin in Type 2 Diabetes Patients: A Randomized, Double-Blind, Placebo-Controlled Study (SOLUTION)
- Byung Wan Lee, KyungWan Min, Eun-Gyoung Hong, Bon Jeong Ku, Jun Goo Kang, Suk Chon, Won-Young Lee, Mi Kyoung Park, Jae Hyeon Kim, Sang Yong Kim, Keeho Song, Soon Jib Yoo
- Endocrinol Metab. 2023;38(3):328-337. Published online June 28, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1688
- 2,416 View
- 264 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
This study evaluated the efficacy and safety of add-on gemigliptin in patients with type 2 diabetes mellitus (T2DM) who had inadequate glycemic control with metformin and dapagliflozin.
Methods
In this randomized, placebo-controlled, parallel-group, double-blind, phase III study, 315 patients were randomized to receive either gemigliptin 50 mg (n=159) or placebo (n=156) with metformin and dapagliflozin for 24 weeks. After the 24-week treatment, patients who received the placebo were switched to gemigliptin, and all patients were treated with gemigliptin for an additional 28 weeks.
Results
The baseline characteristics were similar between the two groups, except for body mass index. At week 24, the least squares mean difference (standard error) in hemoglobin A1c (HbA1c) changes was –0.66% (0.07) with a 95% confidence interval of –0.80% to –0.52%, demonstrating superior HbA1c reduction in the gemigliptin group. After week 24, the HbA1c level significantly decreased in the placebo group as gemigliptin was administered, whereas the efficacy of HbA1c reduction was maintained up to week 52 in the gemigliptin group. The safety profiles were similar: the incidence rates of treatment-emergent adverse events up to week 24 were 27.67% and 29.22% in the gemigliptin and placebo groups, respectively. The safety profiles after week 24 were similar to those up to week 24 in both groups, and no new safety findings, including hypoglycemia, were noted.
Conclusion
Add-on gemigliptin was well tolerated, providing comparable safety profiles and superior efficacy in glycemic control over placebo for long-term use in patients with T2DM who had poor glycemic control with metformin and dapagliflozin.

- Adrenal gland
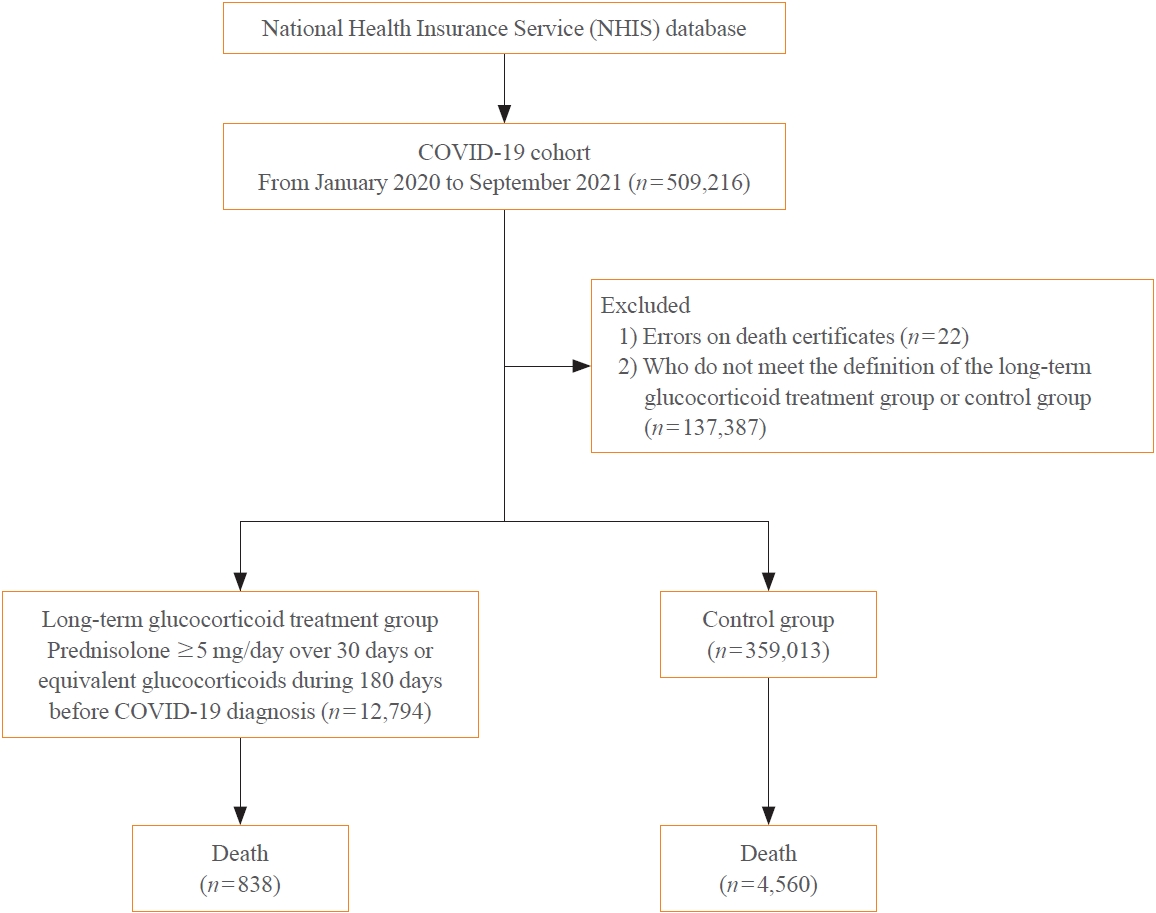
Big Data Articles (National Health Insurance Service Database) - Mortality and Severity of Coronavirus Disease 2019 in Patients with Long-Term Glucocorticoid Therapy: A Korean Nationwide Cohort Study
- Eu Jeong Ku, Keeho Song, Kyoung Min Kim, Gi Hyeon Seo, Soon Jib Yoo
- Endocrinol Metab. 2023;38(2):253-259. Published online March 21, 2023
- DOI: https://doi.org/10.3803/EnM.2022.1607
- 2,634 View
- 103 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The severity of coronavirus disease 2019 (COVID-19) among patients with long-term glucocorticoid treatment (LTGT) has not been established. We aimed to evaluate the association between LTGT and COVID-19 prognosis.
Methods
A Korean nationwide cohort database of COVID-19 patients between January 2019 and September 2021 was used. LTGT was defined as exposure to at least 150 mg of prednisolone (≥5 mg/day and ≥30 days) or equivalent glucocorticoids 180 days before COVID-19 infection. The outcome measurements were mortality, hospitalization, intensive care unit (ICU) admission, length of stay, and mechanical ventilation.
Results
Among confirmed patients with COVID-19, the LTGT group (n=12,794) was older and had a higher proportion of comorbidities than the control (n=359,013). The LTGT group showed higher in-hospital, 30-day, and 90-day mortality rates than the control (14.0% vs. 2.3%, 5.9% vs. 1.1%, and 9.9% vs. 1.8%, respectively; all P<0.001). Except for the hospitalization rate, the length of stay, ICU admission, and mechanical ventilation proportions were significantly higher in the LTGT group than in the control (all P<0.001). Overall mortality was higher in the LTGT group than in the control group, and the significance remained in the fully adjusted model (odds ratio [OR], 5.75; 95% confidence interval [CI], 5.31 to 6.23) (adjusted OR, 1.82; 95% CI, 1.67 to 2.00). The LTGT group showed a higher mortality rate than the control within the same comorbidity score category.
Conclusion
Long-term exposure to glucocorticoids increased the mortality and severity of COVID-19. Prevention and early proactive measures are inevitable in the high-risk LTGT group with many comorbidities. -
Citations
Citations to this article as recorded by- Glucocorticoids as a Double-Edged Sword in the Treatment of COVID-19: Mortality and Severity of COVID-19 in Patients Receiving Long-Term Glucocorticoid Therapy
Eun-Hee Cho
Endocrinology and Metabolism.2023; 38(2): 223. CrossRef - Pituitary Diseases and COVID-19 Outcomes in South Korea: A Nationwide Cohort Study
Jeonghoon Ha, Kyoung Min Kim, Dong-Jun Lim, Keeho Song, Gi Hyeon Seo
Journal of Clinical Medicine.2023; 12(14): 4799. CrossRef
- Glucocorticoids as a Double-Edged Sword in the Treatment of COVID-19: Mortality and Severity of COVID-19 in Patients Receiving Long-Term Glucocorticoid Therapy

- Clinical Study
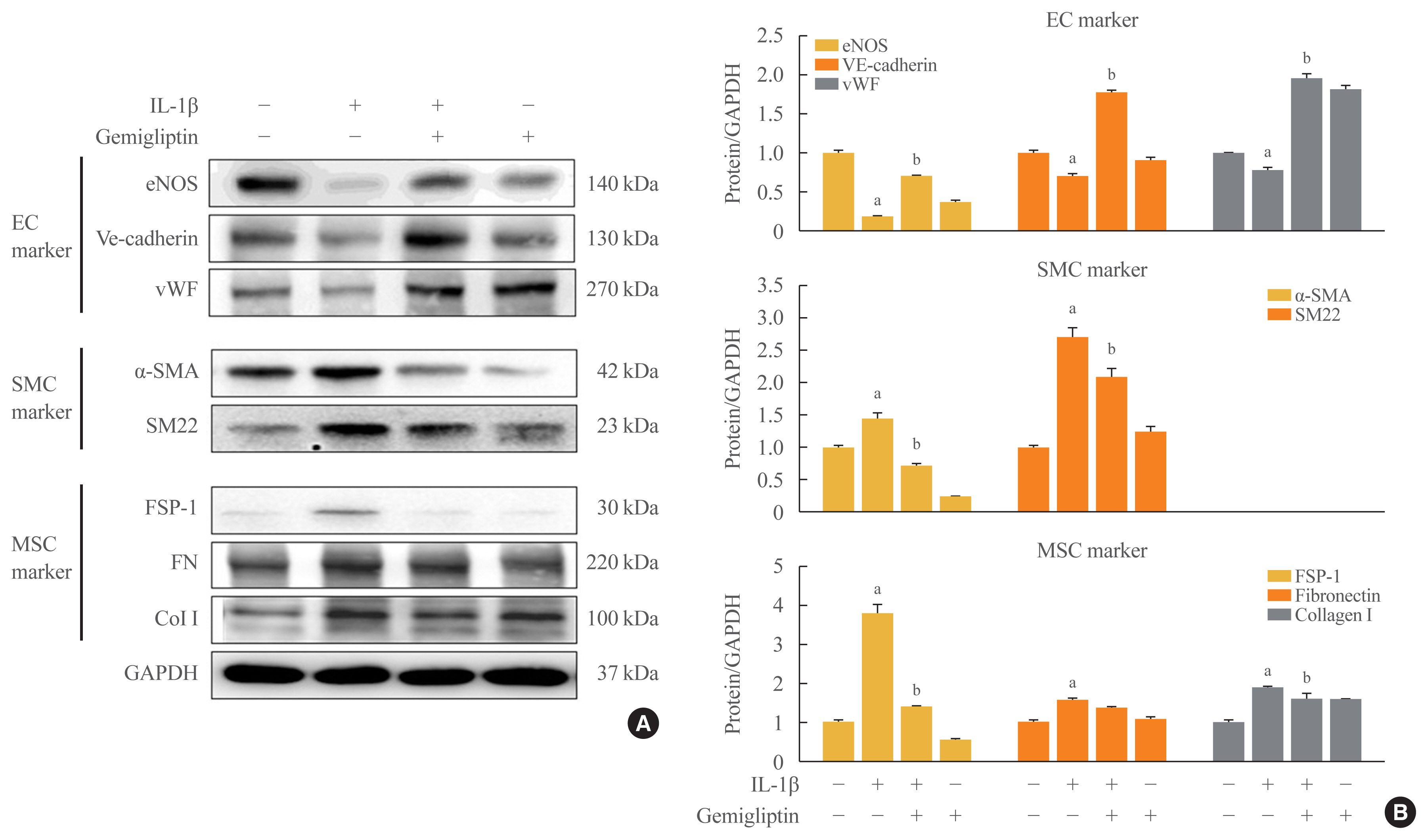
- Gemigliptin Inhibits Interleukin-1β–Induced Endothelial-Mesenchymal Transition via Canonical-Bone Morphogenetic Protein Pathway
- Oak-Kee Hong, Seong-Su Lee, Soon Jib Yoo, Min-Kyung Lee, Mee-Kyoung Kim, Ki-Hyun Baek, Ki-Ho Song, Hyuk-Sang Kwon
- Endocrinol Metab. 2020;35(2):384-395. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.384
- 6,768 View
- 139 Download
- 9 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Endothelial-to-mesenchymal transition (EndMT) contributes to inflammatory conditions inducing conversion of endothelial cells (ECs) into activated fibroblasts, promoting fibrotic diseases. Pro-inflammatory cytokine is the most potent inducer of EndMT. We investigated inhibition of interleukin-1β (IL-1β)-induced EndMT by gemigliptin, a dipeptidyl peptidase-IV inhibitor.
Methods
We exposed human umbilical vein endothelial cells (HUVECs) to 10 ng/mL IL-1β/20 μM gemigliptin and analyzed the expression of endothelial, smooth muscle, mesenchymal, and osteoblastic markers, bone morphogenetic protein (BMP), Smad, and non-Smad signaling pathway proteins.
Results
Morphological changes showed gemigliptin blocked IL-1β-induced EndMT, upregulated EC markers, and downregulated smooth muscle and mesenchymal markers. IL-1β activation of HUVECs is initiated by the BMP/Smad and non-smad BMP signaling pathways. Gemigliptin inhibited IL-1β induction of BMP2 and 7, activin receptor type IA, BMP receptor type IA, and BMP receptor type II. Reversal of IL-1β-mediated inhibition of BMP-induced Smad1/5/8, Smad2, and Smad3 phosphorylation by gemigliptin suggests involvement of the Smad pathway in gemigliptin action. In the non-Smad BMP pathway, gemigliptin treatment significantly increased the deactivation of extracellular regulated protein kinase (ERK), p38, and JNK by IL-1β. Gemigliptin treatment suppressed BMP-2-induced expression of key osteoblastic markers including osterix, runt-related transcription factor 2, and hepcidin during IL-1β-induced EndMT.
Conclusion
We demonstrated a novel protective mechanism of gemigliptin against fibrosis by suppressing IL-1β-induced EndMT. -
Citations
Citations to this article as recorded by- Injured Endothelial Cell: A Risk Factor for Pulmonary Fibrosis
Weiming Zhao, Lan Wang, Yaxuan Wang, Hongmei Yuan, Mengxia Zhao, Hui Lian, Shuaichen Ma, Kai Xu, Zhongzheng Li, Guoying Yu
International Journal of Molecular Sciences.2023; 24(10): 8749. CrossRef - Tissue fibrosis induced by radiotherapy: current understanding of the molecular mechanisms, diagnosis and therapeutic advances
Zuxiang Yu, Chaoyu Xu, Bin Song, Shihao Zhang, Chong Chen, Changlong Li, Shuyu Zhang
Journal of Translational Medicine.2023;[Epub] CrossRef - MiRNAs in Systemic Sclerosis Patients with Pulmonary Arterial Hypertension: Markers and Effectors
Mor Zaaroor Levy, Noa Rabinowicz, Maia Yamila Kohon, Avshalom Shalom, Ariel Berl, Tzipi Hornik-Lurie, Liat Drucker, Shelly Tartakover Matalon, Yair Levy
Biomedicines.2022; 10(3): 629. CrossRef - Recent advance in treatment of atherosclerosis: Key targets and plaque-positioned delivery strategies
Li Li, Sainan Liu, Jianying Tan, Lai Wei, Dimeng Wu, Shuai Gao, Yajun Weng, Junying Chen
Journal of Tissue Engineering.2022; 13: 204173142210885. CrossRef - Vascular Calcification: New Insights Into BMP Type I Receptor A
Zhixing Niu, Guanyue Su, Tiantian Li, Hongchi Yu, Yang Shen, Demao Zhang, Xiaoheng Liu
Frontiers in Pharmacology.2022;[Epub] CrossRef - Yi-Shen-Hua-Shi Granule Alleviates Adriamycin-Induced Glomerular Fibrosis by Suppressing the BMP2/Smad Signaling Pathway
Zhuojing Tan, Yachen Si, Yan Yu, Jiarong Ding, Linxi Huang, Ying Xu, Hongxia Zhang, Yihan Lu, Chao Wang, Bing Yu, Li Yuan
Frontiers in Pharmacology.2022;[Epub] CrossRef - Panax notoginseng Suppresses Bone Morphogenetic Protein-2 Expression in EA.hy926 Endothelial Cells by Inhibiting the Noncanonical NF-κB and Wnt/β-Catenin Signaling Pathways
Tsu-Ni Ping, Shu-Ling Hsieh, Jyh-Jye Wang, Jin-Bor Chen, Chih-Chung Wu
Plants.2022; 11(23): 3265. CrossRef - Vascular calcification: New insights into endothelial cells
Cheng Yuan, Lihua Ni, Changjiang Zhang, Xiaorong Hu, Xiaoyan Wu
Microvascular Research.2021; 134: 104105. CrossRef - Concentrated small extracellular vesicles from menstrual blood-derived stromal cells improve intrauterine adhesion, a pre-clinical study in a rat model
Siwen Zhang, Qiyuan Chang, Pingping Li, Xiaoyu Tong, Yi Feng, Xinyao Hao, Xudong Zhang, Zhengwei Yuan, Jichun Tan
Nanoscale.2021; 13(15): 7334. CrossRef
- Injured Endothelial Cell: A Risk Factor for Pulmonary Fibrosis

- A Case of Pituitary Feedback Adenoma Caused by Primary Hypothyroidism.
- Soon Jib Yoo, Sang A Chang, Yoo Bae Ahn, Hyun Sik Son, Kun Ho Yoon, Moo Il Kang, Bong Yun Cha, Kwang Woo Lee, Ho Young Son, Sung Koo Kang, Myung Hee Chung
- J Korean Endocr Soc. 1996;11(2):199-206. Published online November 7, 2019
- 1,155 View
- 29 Download
-
 Abstract
Abstract
 PDF
PDF - A 14-year-old girl presented with severe headache and grand mal seizure. A magnetic resonance imaging(MRI) of brain showed a pituitary mass(1.0X1.5X1.3cm) incidentally during seizure evaluation. On physical examination, nodular goiter was detected on her anterior neck. The hormone study showed markdly increased basal thyroid stimulating hormone(TSH) level compared to thyroid hormone level, hyperprolactinemia and decreased basal growth hormone level. TSH and prolactin showed exaggerated response to thyrotropin releasing hormone(TRH) and the growth hormone showed delayed and blunted response to insulin-induced hypoglycemia. With the results of thyroid autoantibody and thyroid scan, the diagnosis of Hashimoto's thyroiditis was possible. Thyroid hormone and anticonvulsant drug were started with close observation of clinical status under the impression of pituitary feedback adenoma caused by hypothyroidism. After 3 months replacement therapy of levothyroxine sodium, she achieved euthyroid state with disappearance of headache and nodular goiter. After continuous replacement therapy for 9 months more, the pituitary mass was successfully regressed on follow up MRI with normalization of basal prolactin level. Grand mal seizure was developed after withholding anticonvulsant drug even though continuous admmistration of thyroid hormone. Because of similarity among pituitary adenoma discovered incidentally, careful hormonal study and high index of suspicion should be maintained to achieve correct diagnosis in order to avoid unnecessary pituitary surgery in these patients.

- Clinical Guidelines for the Management of Adrenal Incidentaloma
- Jung-Min Lee, Mee Kyoung Kim, Seung-Hyun Ko, Jung-Min Koh, Bo-Yeon Kim, Sang Wan Kim, Soo-Kyung Kim, Hae Jin Kim, Ohk-Hyun Ryu, Juri Park, Jung Soo Lim, Seong Yeon Kim, Young Kee Shong, Soon Jib Yoo
- Endocrinol Metab. 2017;32(2):200-218. Published online June 23, 2017
- DOI: https://doi.org/10.3803/EnM.2017.32.2.200
- 16,227 View
- 691 Download
- 80 Web of Science
- 78 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader An adrenal incidentaloma is an adrenal mass found in an imaging study performed for other reasons unrelated to adrenal disease and often accompanied by obesity, diabetes, or hypertension. The prevalence and incidence of adrenal incidentaloma increase with age and are also expected to rise due to the rapid development of imaging technology and frequent imaging studies. The Korean Endocrine Society is promoting an appropriate practice guideline to meet the rising incidence of adrenal incidentaloma, in cooperation with the Korean Adrenal Gland and Endocrine Hypertension Study Group. In this paper, we discuss important core issues in managing the patients with adrenal incidentaloma. After evaluating core proposition, we propose the most critical 20 recommendations from the initially organized 47 recommendations by Delphi technique.
-
Citations
Citations to this article as recorded by- The improvement of postoperative blood pressure and associated factors in patients with hormone‐negative adrenal adenoma and hypertension
Jiaxing Sun, Yingchun Dong, Hanbo Wang, Xudong Guo, Ning Suo, Shangjian Li, Xiangbin Ren, Shaobo Jiang
Journal of Surgical Oncology.2024; 129(6): 1073. CrossRef - Clinical features and treatment options for pediatric adrenal incidentalomas: a retrospective single center study
Xiaojiang Zhu, Saisai Liu, Yimin Yuan, Nannan Gu, Jintong Sha, Yunfei Guo, Yongji Deng
BMC Pediatrics.2024;[Epub] CrossRef - Characterizing incidental mass lesions in abdominal dual-energy CT compared to conventional contrast-enhanced CT
Jack Junchi Xu, Peter Sommer Ulriksen, Camilla Wium Bjerrum, Michael Patrick Achiam, Timothy Andrew Resch, Lars Lönn, Kristoffer Lindskov Hansen
Acta Radiologica.2023; 64(3): 945. CrossRef - Metastatic Adrenal PEComa: Case Report and Short Review of the Literature
Enrico Battistella, Luca Pomba, Marica Mirabella, Michele Gregianin, Antonio Scapinello, Marco Volante, Antonio Toniato
Medicina.2023; 59(1): 149. CrossRef - Surgical management and outcomes of spinal metastasis of malignant adrenal tumor: A retrospective study of six cases and literature review
Xiangzhi Ni, Jing Wang, Jiashi Cao, Kun Zhang, Shuming Hou, Xing Huang, Yuanjin Song, Xin Gao, Jianru Xiao, Tielong Liu
Frontiers in Oncology.2023;[Epub] CrossRef - An adrenal incidentaloma that had appeared to produce dehydroepiandrosterone-sulfate in excess before immunohistochemical study of the tumor
Toshihide Yamamoto, Takuma Kimura, Yuki Kubo, Shin-ichi Nakatsuka, Hiromasa Harada, Takashi Suzuki, Hironobu Sasano
Endocrine Journal.2023; 70(1): 43. CrossRef - Mortality Not Increased in Patients With Nonfunctional Adrenal Adenomas: A Matched Cohort Study
Albin Kjellbom, Ola Lindgren, Malin Danielsson, Henrik Olsen, Magnus Löndahl
The Journal of Clinical Endocrinology & Metabolism.2023; 108(8): e536. CrossRef - Construction of a novel clinical nomogram to predict cancer-specific survival in patients with primary malignant adrenal tumors: a large population-based retrospective study
Mingzhen Li, Xiaoying Duan, Di You, Linlin Liu
Frontiers in Medicine.2023;[Epub] CrossRef - Primary Aldosteronism Prevalence – An Unfolding
Story
Suranut Charoensri, Adina F. Turcu
Experimental and Clinical Endocrinology & Diabetes.2023; 131(07/08): 394. CrossRef - Management of Adrenal Cortical Adenomas: Assessment of Bone Status in Patients with (Non-Functioning) Adrenal Incidentalomas
Alexandra-Ioana Trandafir, Mihaela Stanciu, Simona Elena Albu, Vasile Razvan Stoian, Irina Ciofu, Cristian Persu, Claudiu Nistor, Mara Carsote
Journal of Clinical Medicine.2023; 12(13): 4244. CrossRef - Clinical manifestations of functionally autonomous cortisol secretion in patients with adrenal masse
T. R. Chzhen, T. P. Kiseleva
Ural Medical Journal.2023; 22(3): 13. CrossRef - Tumor enlargement in adrenal incidentaloma is related to glaucoma: a new prognostic feature?
M. Caputo, T. Daffara, A. Ferrero, M. Romanisio, E. Monti, C. Mele, M. Zavattaro, S. Tricca, A. Siani, A. Clemente, C. Palumbo, S. De Cillà, A. Carriero, A. Volpe, P. Marzullo, G. Aimaretti, F. Prodam
Journal of Endocrinological Investigation.2023; 47(2): 377. CrossRef - Adrenal ganglioneuroma: Features and outcomes of cases series
Pei Li, Rongchang Zhang, Guang Wang, Jiongming Li
Asian Journal of Surgery.2023; 46(11): 5272. CrossRef - Recent Updates on the Management of Adrenal Incidentalomas
Seung Shin Park, Jung Hee Kim
Endocrinology and Metabolism.2023; 38(4): 373. CrossRef - Adrenal malakoplakia a rare lesion that mimics a neoplasm
Orión Erenhú Rodríguez González, Jesus Eduardo Osorio, Edgar Iván Bravo Castro
Urology Case Reports.2023; 51: 102568. CrossRef - LC-MS based simultaneous profiling of adrenal hormones of steroids, catecholamines, and metanephrines
Jongsung Noh, Chaelin Lee, Jung Hee Kim, Seung Woon Myung, Man Ho Choi
Journal of Lipid Research.2023; 64(11): 100453. CrossRef - Incidentaloma adrenal. Del hallazgo casual al diagnóstico definitivo
Mercedes Retamal Ortíz, Ana Belén Vicario Parada, Elena Vázquez Jarén
Actualización en Medicina de Familia.2023;[Epub] CrossRef - Diagnosis and management of adrenal incidentaloma: use of clinical judgment and evidence in dialog with the patient
Yusaku Yoshida, Kiyomi Horiuchi, Michio Otsuki, Takahiro Okamoto
Surgery Today.2023;[Epub] CrossRef - Can MDCT Enhancement Patterns Be Helpful in Differentiating Secretory from Non-Functional Adrenal Adenoma?
Svetlana Kocic, Vladimir Vukomanovic, Aleksandar Djukic, Jovica Saponjski, Dusan Saponjski, Vuk Aleksic, Vesna Ignjatovic, Katarina Vuleta Nedic, Vladan Markovic, Radisa Vojinovic
Medicina.2023; 60(1): 72. CrossRef - Computer-assisted Reporting and Decision Support Increases Compliance with Follow-up Imaging and Hormonal Screening of Adrenal Incidentalomas
Renata R. Almeida, Bernardo C. Bizzo, Ramandeep Singh, Katherine P. Andriole, Tarik K. Alkasab
Academic Radiology.2022; 29(2): 236. CrossRef - Incidental Adrenal Masses: Adherence to Guidelines and Methods to Improve Initial Follow-Up: A Systematic Review
Timothy Feeney, Andrea Madiedo, Philip E. Knapp, Avneesh Gupta, David McAneny, Frederick Thurston Drake
Journal of Surgical Research.2022; 269: 18. CrossRef - Incidental Adrenal Lesions May Not Always Require Further Imaging Work-up
Deborah A. Baumgarten
Radiology.2022; 302(1): 138. CrossRef - Adrenal Nodules Detected at Staging CT in Patients with Resectable Gastric Cancers Have a Low Incidence of Malignancy
Hae Young Kim, Won Chang, Yoon Jin Lee, Ji Hoon Park, Jungheum Cho, Hee Young Na, Hyungwoo Ahn, Sung Il Hwang, Hak Jong Lee, Young Hoon Kim, Kyoung Ho Lee
Radiology.2022; 302(1): 129. CrossRef - Management of incidental adrenal nodules: a survey of abdominal radiologists conducted by the Society of Abdominal Radiology Disease-Focused Panel on Adrenal Neoplasms
Michael T. Corwin, Nicola Schieda, Erick M. Remer, Elaine M. Caoili
Abdominal Radiology.2022; 47(4): 1360. CrossRef - Primary hyperaldosteronism: indications for screening
Novella M. Chikhladze
Terapevticheskii arkhiv.2022; 94(1): 107. CrossRef - Pathophysiological Link between Insulin Resistance and Adrenal Incidentalomas
Jordan A. Higgs, Alyssa P. Quinn, Kevin D. Seely, Zeke Richards, Shad P. Mortensen, Cody S. Crandall, Amanda E. Brooks
International Journal of Molecular Sciences.2022; 23(8): 4340. CrossRef - Can Radiomics Provide Additional Diagnostic Value for Identifying Adrenal Lipid-Poor Adenomas From Non-Adenomas on Unenhanced CT?
Binhao Zhang, Huangqi Zhang, Xin Li, Shengze Jin, Jiawen Yang, Wenting Pan, Xue Dong, Jin Chen, Wenbin Ji
Frontiers in Oncology.2022;[Epub] CrossRef - Adrenal Surgery in the Era of Multidisciplinary Endocrine Tumor
Boards
Costanza Chiapponi, Daniel Pinto Dos Santos, Milan Janis Michael Hartmann, Matthias Schmidt, Michael Faust, Roger Wahba, Christiane Josephine Bruns, Anne Maria Schultheis, Hakan Alakus
Hormone and Metabolic Research.2022; 54(05): 294. CrossRef - Optimal and novel imaging of the adrenal glands
Patrick J. Navin, Michael R. Moynagh
Current Opinion in Endocrinology, Diabetes & Obesity.2022; 29(3): 253. CrossRef - Adrenal Tumors in Young Adults: Case Reports and Literature Review
Małgorzata Zdrojewska, Emilia Mech-Siebieszuk, Renata Świątkowska-Stodulska, Bartosz Regent, Michał Kunc, Łukasz Zdrojewski, Krzysztof Sworczak
Medicina.2022; 58(6): 746. CrossRef - Incidence of malignancy in adrenal nodules detected on staging CTs of patients with potentially resectable colorectal cancer
Hae Young Kim, Yoon Jin Lee, Won Chang, Ji Hoon Park, Jungheum Cho, Hyeon Jeong Oh, Young Hoon Kim, Kyoung Ho Lee
European Radiology.2022; 32(12): 8560. CrossRef - Appendiceal Incidentalomas: Prevalence, Radiographic Characteristics, Management, and Outcomes
Adam Kelly, Stacy O’Connor, Diana Kane, Chiang-Ching Huang, Harveshp Mogal
Annals of Surgical Oncology.2022; 29(13): 8265. CrossRef - Laparoscopic large adrenal mass resection: why we should be more careful?
Mohsen Varyani, Mahmood Parvin, Hamidreza Akbari Gilani
African Journal of Urology.2022;[Epub] CrossRef - Serum Visfatin/NAMPT as a Potential Risk Predictor for Malignancy of Adrenal Tumors
Nadia Sawicka-Gutaj, Hanna Komarowska, Dawid Gruszczyński, Aleksandra Derwich, Anna Klimont, Marek Ruchała
Journal of Clinical Medicine.2022; 11(19): 5563. CrossRef - Application of radiomics in adrenal incidentaloma: a literature review
Cheng Li, Yan Fu, Xiaoping Yi, Xiao Guan, Longfei Liu, Bihong T. Chen
Discover Oncology.2022;[Epub] CrossRef - Hormone-inactive adrenal tumors in clinician’s practice
T. R. Chzhen, T. P. Kiseleva
Perm Medical Journal.2022; 39(5): 48. CrossRef - The diagnostic value of salivary cortisol and salivary cortisone in patients with suspected hypercortisolism
Vendela Berndt, Per Dahlqvist, Jennie de Verdier, Henrik Ryberg, Oskar Ragnarsson
Frontiers in Endocrinology.2022;[Epub] CrossRef - The Role of Intraoperative Indocyanine Green (ICG) and Preoperative 3-Dimensional (3D) Reconstruction in Laparoscopic Adrenalectomy: A Propensity Score-matched Analysis
Giuseppe Palomba, Vincenza Paola Dinuzzi, Francesca Pegoraro, Roberto Ivan Troisi, Roberto Montalti, Giovanni Domenico De Palma, Giovanni Aprea
Surgical Laparoscopy, Endoscopy & Percutaneous Techniques.2022; 32(6): 643. CrossRef - The Etiological Profile of Adrenal Incidentalomas
Fatima-Zahra Lahmamssi, Loubna Saadaoui, Hayat Aynaou, Houda Salhi, Hanan El Ouahabi
Cureus.2022;[Epub] CrossRef - Forty Years Together, New Leap Forward! The 40th Anniversary of the Korean Endocrine Society
Jong Chul Won, Ki-Hyun Baek
Endocrinology and Metabolism.2022; 37(6): 851. CrossRef - Conduite à tenir face à un fortuitome surrénalien chez le chien ou le chat
Diane Pichard, Ghita Benckekroun
Le Nouveau Praticien Vétérinaire canine & féline.2022; 19(82): 40. CrossRef - Laparoscopic transperitoneal adrenalectomy: a comparative study of different techniques for vessel sealing
Luca Cardinali, Edlira Skrami, Elisa Catani, Flavia Carle, Monica Ortenzi, Andrea Balla, Mario Guerrieri
Surgical Endoscopy.2021; 35(2): 673. CrossRef - Epidemiology and Comorbidity of Adrenal Cushing Syndrome: A Nationwide Cohort Study
Chang Ho Ahn, Jung Hee Kim, Man Young Park, Sang Wan Kim
The Journal of Clinical Endocrinology & Metabolism.2021; 106(3): e1362. CrossRef - Urine steroid profile as a new promising tool for the evaluation of adrenal tumors. Literature review
Marta Araujo-Castro, Pablo Valderrábano, Héctor F. Escobar-Morreale, Felicia A. Hanzu, Gregori Casals
Endocrine.2021; 72(1): 40. CrossRef - A Rare Neoplasm: Primary Adrenal Leiomyosarcoma
Jack T. Barnett, Christine W. Liaw, Reza Mehrazin
Urology.2021; 148: e11. CrossRef - Adrenal Ganglioneuroma Presenting as an Incidentaloma in an Adolescent Patient
Sonia G. Sharma, Steven N. Levine, Xin Gu
AACE Clinical Case Reports.2021; 7(1): 61. CrossRef - Feasibility of Iodine-131 6β-Methyl-Iodo-19 Norcholesterol (NP-59) Scintigraphy to Complement Adrenal Venous Sampling in Management of Primary Aldosteronism: A Case Series
Jeongmin Lee, Jeonghoon Ha, Sang-Kuon Lee, Hye Lim Park, Sung-Hoon Kim, Dong-Jun Lim, Jung Min Lee, Sang-Ah Chang, Moo Il Kang, Min-Hee Kim
International Journal of General Medicine.2021; Volume 14: 673. CrossRef - Best Achievements in Pituitary and Adrenal Diseases in 2020
Chang Ho Ahn, Jung Hee Kim
Endocrinology and Metabolism.2021; 36(1): 51. CrossRef - Adrenal surgery: Review of 35 years experience in a single centre
Enrico Battistella, Stefania Ferrari, Luca Pomba, Antonio Toniato
Surgical Oncology.2021; 37: 101554. CrossRef - Adrenocortical Carcinoma: A Case of Missed Diagnosis
Yusef Hazimeh, Carlie Sigel, Carsello Carie, Mathew Leinung, Zaynab Khalaf
Cureus.2021;[Epub] CrossRef - Imagerie fonctionnelle en endocrinologie : nouveaux paradigmes à l’horizon 2020
E. Marchal
Médecine Nucléaire.2021; 45(3): 158. CrossRef - Adrenal Incidentaloma
Caren G. Solomon, Electron Kebebew
New England Journal of Medicine.2021; 384(16): 1542. CrossRef - Can Hematological Parameters Play a Role in the Differential Diagnosis of Adrenal Tumors?
Mehmet Gürkan Arıkan, Göktan Altuğ Öz, Nur Gülce İşkan, Necdet Süt, İlkan Yüksel, Ersan Arda
Uro.2021; 1(2): 39. CrossRef - Incidental Adrenal Nodules
Daniel I. Glazer, Michael T. Corwin, William W. Mayo-Smith
Radiologic Clinics of North America.2021; 59(4): 591. CrossRef - Antioxidant Barrier and Oxidative Damage to Proteins, Lipids, and DNA/RNA in Adrenal Tumor Patients
Barbara Choromańska, Piotr Myśliwiec, Tomasz Kozłowski, Magdalena Łuba, Piotr Wojskowicz, Jacek Dadan, Hanna Myśliwiec, Katarzyna Choromańska, Anna Gibała, Anna Starzyńska, Małgorzata Żendzian-Piotrowska, Anna Zalewska, Mateusz Maciejczyk, Jos L. Quiles
Oxidative Medicine and Cellular Longevity.2021; 2021: 1. CrossRef - Laparoscopic Retroperitoneoscopic Removal of an Adrenal Hemangioma: a Case Report
Kristin McCoy, Katherine Howe, Daniel Tershak
Journal of Endocrine Surgery.2021; 21(3): 70. CrossRef - Metabolic Subtyping of Adrenal Tumors: Prospective Multi-Center Cohort Study in Korea
Eu Jeong Ku, Chaelin Lee, Jaeyoon Shim, Sihoon Lee, Kyoung-Ah Kim, Sang Wan Kim, Yumie Rhee, Hyo-Jeong Kim, Jung Soo Lim, Choon Hee Chung, Sung Wan Chun, Soon-Jib Yoo, Ohk-Hyun Ryu, Ho Chan Cho, A Ram Hong, Chang Ho Ahn, Jung Hee Kim, Man Ho Choi
Endocrinology and Metabolism.2021; 36(5): 1131. CrossRef - Cross-Talk Between Nitrosative Stress, Inflammation and Hypoxia-Inducible Factor in Patients with Adrenal Masses
Barbara Choromańska, Piotr Myśliwiec, Tomasz Kozłowski, Magdalena Łuba, Piotr Wojskowicz, Jacek Dadan, Hanna Myśliwiec, Katarzyna Choromańska, Katarzyna Makarewicz, Anna Zalewska, Mateusz Maciejczyk
Journal of Inflammation Research.2021; Volume 14: 6317. CrossRef - Cirugía laparoscópica en incidentaloma suprarrenal para el cirujano general: serie de casos
Martín Adrián Bolívar-Rodríguez, Marcel Antonio Cázarez-Aguilar, Pedro Alejandro Magaña-Zavala, Francisco Magaña-Olivas, José Martín Niebla-Moreno
Revista Mexicana de Cirugía Endoscópica.2021; 22(1): 8. CrossRef - Adrenal adenomas: what to do with them? Review 2
S. Rybakov
INTERNATIONAL JOURNAL OF ENDOCRINOLOGY (Ukraine).2021; 17(3): 241. CrossRef - Is Follow-up of Adrenal Incidentalomas Always Mandatory?
Giuseppe Reimondo, Alessandra Muller, Elisa Ingargiola, Soraya Puglisi, Massimo Terzolo
Endocrinology and Metabolism.2020; 35(1): 26. CrossRef - Imaging Findings of Primary Adrenal Leiomyosarcoma: A Case Report
Hye Ran Yoon, Dong Hee Park
Journal of the Korean Society of Radiology.2020; 81(2): 459. CrossRef - WFUMB position paper on the management incidental findings: adrenal incidentaloma
Christoph F. Dietrich, Jean Michel Correas, Yi Dong, Christian Nolsoe, Susan Campbell Westerway, Christian Jenssen
Ultrasonography.2020; 39(1): 11. CrossRef - A nationwide survey of adrenal incidentalomas in Japan: the first report of clinical and epidemiological features
Takamasa Ichijo, Hajime Ueshiba, Hajime Nawata, Toshihiko Yanase
Endocrine Journal.2020; 67(2): 141. CrossRef - Mimics, pitfalls, and misdiagnoses of adrenal masses on CT and MRI
Khaled M. Elsayes, Mohab M. Elmohr, Sanaz Javadi, Christine O. Menias, Erick M. Remer, Ajaykumar C. Morani, Akram M. Shaaban
Abdominal Radiology.2020; 45(4): 982. CrossRef - Adrenal Incidentaloma
Mark Sherlock, Andrew Scarsbrook, Afroze Abbas, Sheila Fraser, Padiporn Limumpornpetch, Rosemary Dineen, Paul M Stewart
Endocrine Reviews.2020; 41(6): 775. CrossRef - A Web Application for Adrenal Incidentaloma Identification, Tracking, and Management Using Machine Learning
Wasif Bala, Jackson Steinkamp, Timothy Feeney, Avneesh Gupta, Abhinav Sharma, Jake Kantrowitz, Nicholas Cordella, James Moses, Frederick Thurston Drake
Applied Clinical Informatics.2020; 11(04): 606. CrossRef - Presentation and outcome of patients with an adrenal mass: A retrospective observational study
Nadeema Rafiq, Tauseef Nabi, SajadAhmad Dar, Shahnawaz Rasool
Clinical Cancer Investigation Journal.2020; 9(5): 198. CrossRef - Evaluation of Functionality and Growth Rates in Adrenal Incidentalomas: Single Center Experience
Suna AVCI, Yüksel Aslı OZTURKMEN, Sayid ZUHUR, Gulkan OZKAN, Elif GUVEN, Nazan DEMİR, Yuksel ALTUNTAS
Phoenix Medical Journal.2020; 2(3): 125. CrossRef - Percutaneous Adrenal Radiofrequency Ablation: A Short Review for Endocrinologists
Byung Kwan Park
Endocrinology and Metabolism.2020; 35(4): 750. CrossRef - Autonomous cortisol secretion in adrenal incidentalomas
Marta Araujo-Castro, Miguel Antonio Sampedro Núñez, Mónica Marazuela
Endocrine.2019; 64(1): 1. CrossRef - Primary adrenal schwannoma: a series of 31 cases emphasizing their clinicopathologic features and favorable prognosis
Jun Zhou, Dandan Zhang, Wencai Li, Luting Zhou, Haimin Xu, Saifang Zheng, Chaofu Wang
Endocrine.2019; 65(3): 662. CrossRef - Challenging risk factors for right and left laparoscopic adrenalectomy: A single centre experience with 272 cases
Kadir Omur Gunseren, Mehmet Cagatay Cicek, Hakan Vuruskan, Yakup Kordan, Ismet Yavascaoglu
International braz j urol.2019; 45(4): 747. CrossRef - A case report on 111In chloride bone marrow scintigraphy in management of adrenal myelolipoma
Tatsuya Yamamoto, Mitsuru Koizumi, Atsushi Kohno, Noboru Numao, Kentaro Inamura
Medicine.2019; 98(8): e14625. CrossRef - PRACTICAL ASPECTS OF LAPAROSCOPIC ADRENALECTOMY IN CHILDREN WITH BENIGN ADRENAL TUMORS
I. V. Poddubny, R. S. Oganesyan, K. N. Tolstov, M. A. Kareva
Russian Journal of Pediatric Surgery.2019; 23(5): 248. CrossRef - Incidental neuroblastoma with bilateral retinoblastoma: what are the chances?
Kelsey Roelofs, Furqan Shaikh, William Astle, Brenda L. Gallie, Sameh E. Soliman
Ophthalmic Genetics.2018; 39(3): 410. CrossRef - Surgical Considerations in Subclinical Cushing’s Syndrome. When is it Time to Operate?
Alexander M. Nixon, C Aggeli, C Tserkezis, GN Zografos
Hellenic Journal of Surgery.2018; 90(1): 27. CrossRef - Adrenal incidentaloma – diagnostic and treating problem – own experience
Ryszard Pogorzelski, Krzysztof Celejewski, Sadegh Toutounchi, Ewa Krajewska, Tomasz Wołoszko, Małgorzata Szostek, Wawrzyniec Jakuczun, Patryk Fiszer, Małgorzata Legocka, Zbigniew Gałązka
Open Medicine.2018; 13(1): 281. CrossRef
- The improvement of postoperative blood pressure and associated factors in patients with hormone‐negative adrenal adenoma and hypertension

- Obesity and Metabolism
- Two Cases of Allergy to Insulin in Gestational Diabetes
- Gi Jun Kim, Shin Bum Kim, Seong Il Jo, Jin Kyeong Shin, Hee Sun Kwon, Heekyung Jeong, Jang Won Son, Seong Su Lee, Sung Rae Kim, Byung Kee Kim, Soon Jib Yoo
- Endocrinol Metab. 2015;30(3):402-407. Published online May 18, 2015
- DOI: https://doi.org/10.3803/EnM.2015.30.3.402
- 4,860 View
- 60 Download
- 3 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Allergic reaction to insulin is uncommon since the introduction of human recombinant insulin preparations and is more rare in pregnant than non-pregnant females due to altered immune reaction during pregnancy. Herein, we report two cases of allergic reaction to insulin in gestational diabetes that were successfully managed. One case was a 33-year-old female using isophane-neutral protamine Hagedorn human insulin and insulin lispro. She experienced dyspnea, cough, urticaria and itching sensation at the sites of insulin injection immediately after insulin administration. We discontinued insulin therapy and started oral hypoglycemic agents with metformin and glibenclamide. The other case was a 32-year-old female using insulin lispro and insulin detemer. She experienced pruritus and burning sensation and multiple nodules at the sites of insulin injection. We changed the insulin from insulin lispro to insulin aspart. Assessments including immunoglobulin E (IgE), IgG, eosinophil, insulin antibody level and skin biopsy were performed. In the two cases, the symptoms were resolved after changing the insulin to oral agents or other insulin preparations. We report two cases of allergic reaction to human insulin in gestational diabetes due to its rarity.
-
Citations
Citations to this article as recorded by- Non-glycemic Adverse Effects of Insulin
Alissa M. Guarneri , Robert P. Hoffman
Current Diabetes Reviews.2022;[Epub] CrossRef - Faulty Injection Technique: A Preventable But Often Overlooked Factor in Insulin Allergy
Partha Pratim Chakraborty, Sugata Narayan Biswas, Shinjan Patra
Diabetes Therapy.2016; 7(1): 163. CrossRef
- Non-glycemic Adverse Effects of Insulin

- Obesity and Metabolism
- Olanzapine-Induced Diabetic Ketoacidosis and Neuroleptic Malignant Syndrome with Rhabdomyolysis: A Case Report
- Young Kyoung Sa, Hyeon Yang, Hee Kyoung Jung, Jang Won Son, Seong Su Lee, Seong Rae Kim, Bong Yeon Cha, Ho Young Son, Chi-Un Pae, Soon Jib Yoo
- Endocrinol Metab. 2013;28(1):70-75. Published online March 25, 2013
- DOI: https://doi.org/10.3803/EnM.2013.28.1.70
- 3,931 View
- 37 Download
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Atypical antipsychotics have replaced conventional antipsychotics in the treatment of schizophrenia because they have less of a propensity to cause undesirable neurologic adverse events including extrapyramidal symptoms, tardive dyskinesia, and neuroleptic malignant syndrome (NMS). However, atypical antipsychotics have been known to result in various metabolic complications such as impaired glucose tolerance, diabetes and even diabetic ketoacidosis (DKA). In addition, a number of NMS cases have been reported in patients treated with atypical antipsychotics, although the absolute incidence of neurologic side effects is currently significantly low. Here, we report a patient who simultaneously developed DKA, acute renal failure and NMS with rhabdomyolysis after olanzapine treatment. Olanzapine-induced metabolic complications and NMS were dramatically improved with cessation of the olanzapine treatment and initiation of supportive management including fluid therapy, hemodialysis, and intensive glycemic control using insulin. At short-term follow-up, insulin secretion was markedly recovered as evidenced by a restoration of serum C-peptide level, and the patient no longer required any hypoglycemic medications. Despite the dramatic increase in the use of atypical antipsychotics treatment, individualized treatments along with careful monitoring may be prudent for high risk or vulnerable patients in order to avoid the development of metabolic side effects.
-
Citations
Citations to this article as recorded by- Neuroleptic malignant syndrome in a patient with moderate intellectual disability treated with olanzapine: A case report
Francesco Piacenza, Suet Kee Ong, Patrick O’Brien, Maurice Clancy
Clinical Case Reports.2021; 9(4): 2404. CrossRef - Succinylcholine-Induced Rhabdomyolysis in Adults: Case Report and Review of the Literature
Robert William Barrons, Liem T. Nguyen
Journal of Pharmacy Practice.2020; 33(1): 102. CrossRef - Improvement in renal prognosis with prompt hemodialysis in hyperosmolar hyperglycemic state-related rhabdomyolysis
I-Wen Chen, Cheng-Wei Lin
Medicine.2018; 97(50): e13647. CrossRef - Treatment of Diabetic Ketoacidosis Associated With Antipsychotic Medication
Antonia Vuk, Maja Baretic, Martina Matovinovic Osvatic, Igor Filipcic, Nikolina Jovanovic, Martina Rojnic Kuzman
Journal of Clinical Psychopharmacology.2017; 37(5): 584. CrossRef - A Case of Primary Hypoparathyroidism Presenting with Acute Kidney Injury Secondary to Rhabdomyolysis
Abdullah Sumnu, Zeki Aydin, Meltem Gursu, Sami Uzun, Serhat Karadag, Egemen Cebeci, Savas Ozturk, Rumeyza Kazancioglu
Case Reports in Nephrology.2016; 2016: 1. CrossRef - Nanoneurotherapeutics approach intended for direct nose to brain delivery
Shadab Md, Gulam Mustafa, Sanjula Baboota, Javed Ali
Drug Development and Industrial Pharmacy.2015; 41(12): 1922. CrossRef - Brief Review of Articles in 'Endocrinology and Metabolism' in 2013
Won-Young Lee
Endocrinology and Metabolism.2014; 29(3): 251. CrossRef
- Neuroleptic malignant syndrome in a patient with moderate intellectual disability treated with olanzapine: A case report

- Characterization of Incidentally Detected Adrenal Pheochromocytoma.
- Soon Jib Yoo, Woohyeon Kim
- Endocrinol Metab. 2012;27(2):116-118. Published online June 20, 2012
- DOI: https://doi.org/10.3803/EnM.2012.27.2.116
- 1,599 View
- 19 Download

- Pharmacological Treatment of Obesity.
- Soon Jib Yoo
- J Korean Endocr Soc. 2008;23(4):223-233. Published online August 1, 2008
- DOI: https://doi.org/10.3803/jkes.2008.23.4.223
- 1,713 View
- 24 Download
- 12 Crossref
-
 Abstract
Abstract
 PDF
PDF - No abstract available.
-
Citations
Citations to this article as recorded by- Study on the Criteria for Priority-Setting and Application in Expanding Health Insurance Benefit of Preventive Medical Service: The Case of Obesity
Gyuwon Ra, Sunmi Lee
Korean Journal of Family Practice.2023; 13(2): 88. CrossRef - Effect of Complex Korean Medicine Treatment on Obese Patient: A Retrospective Study
Byung Jun Kim, Eun Jung Lee, Young Jin Kim, Won Hae Ku, Won Gu Lee, Ki Byoung Kim, Min Seok Oh
Journal of Korean Medicine for Obesity Research.2022; 22(1): 47. CrossRef - Effects of Cabbage-Apple Juice Fermented by Lactobacillus plantarum EM on Lipid Profile Improvement and Obesity Amelioration in Rats
Sihoon Park, Hee-Kyoung Son, Hae-Choon Chang, Jae-Joon Lee
Nutrients.2020; 12(4): 1135. CrossRef - Anti-oxidant and anti-adipocyte differentiation ofAster glehniandAster yomena
Ji Yeon Lee, Jeong-Yong Park, Hyung Don Kim, Seung Eun Lee, Jeong Hoon Lee, Yunji Lee, Kyung Hye Seo
Journal of Nutrition and Health.2019; 52(3): 250. CrossRef - Enhancement of Anti-Obesity Activities of Aronia melanocarpa Elliot Extracts from Low Temperature Ultrasonification Process
Nam Young Kim, Jeong Min Lee, Jae Yong Lee, Hyeon Yong Lee
Korean Journal of Medicinal Crop Science.2016; 24(4): 309. CrossRef - Weight loss effects of Bariatric Surgery after nutrition education in extremely obese patients*
Eun-Ha Jeong, Hong-Chan Lee, Jung-Eun Yim
Journal of Nutrition and Health.2015; 48(1): 30. CrossRef - Suppressive Effect of Acorn (Quercus acutissima Carr.) Extracts in 3T3-L1 Preadipocytes
Ji-Yeon Kim, Jin Lee, Chang-Won Lee, Ae-Jung Kim
The Korean Journal of Food And Nutrition.2015; 28(4): 650. CrossRef - Lemon detox diet reduced body fat, insulin resistance, and serum hs-CRP level without hematological changes in overweight Korean women
Mi Joung Kim, Jung Hyun Hwang, Hyun Ji Ko, Hye Bock Na, Jung Hee Kim
Nutrition Research.2015; 35(5): 409. CrossRef - Weight loss effects of Bariatric Surgery after nutrition education in extremely obese patients*
Eun-Ha Jeong, Hong-Chan Lee, Jung-Eun Yim
Journal of Nutrition and Health.2015; 48(1): 30. CrossRef - Effect of Probiotics-Fermented Samjunghwan on Differentiation in 3T3-L1 Preadipocytes
Mi-Young Song, Shambhunath Bose, Ho-Jun Kim
Journal of the Korean Society of Food Science and Nutrition.2013; 42(1): 1. CrossRef - Effects of CJB Water Extract on Obesity-Related Factors in Hypothalamus of Rats Fed High-Fat Diet
Jeong-Soo Hwang, Jang-Mi Suk, Hye-Min Choi, In-Soon Shin, Su-Jung Hwang, Ji-Young Park, Sung-Ok Kim, Bu-Il Seo, Mi-Ryeo Kim
The Korea Journal of Herbology.2012; 27(5): 99. CrossRef - Effects of Weight Control Program on Dietary Habits and Blood Composition in Obese Middle-Aged Women
Hye-Kyung Kim, Mi-Jeong Kim
The Korean Journal of Nutrition.2010; 43(3): 273. CrossRef
- Study on the Criteria for Priority-Setting and Application in Expanding Health Insurance Benefit of Preventive Medical Service: The Case of Obesity

- A Case of Lymphocytic Infundibuloneurohypophysitis Along with Central Diabetes Insipidus, and this Improved with Conservative Care.
- Ji Myoung Lee, Sang Mi Park, Byung Hee Hwang, Hyun Sook Choi, Seong Su Lee, Jee Young Kim, Sung Rae Kim, Kwang Woo Lee, Ho Young Son, Sung Koo Kang, Soon Jib Yoo
- J Korean Endocr Soc. 2008;23(2):142-147. Published online April 1, 2008
- DOI: https://doi.org/10.3803/jkes.2008.23.2.142
- 1,846 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - Idiopathic central diabetes insipidus is most likely to occur in young patients who have a clinical history of autoimmune disease. The presentation of clinical findings such as central diabetes insipidus and pituitary stalk thickening on sellar magnetic resonance imaging (MRI) in a young women would strongly suggest lymphocytic hypophysitis, which is a rare inflammatory process involving the pituitary stalk and the pituitary gland, yet this disease can sometimes regress.

- Aldosterone as a Cardiovascular Risk Factor.
- Soon Jib Yoo
- J Korean Endocr Soc. 2007;22(1):8-10. Published online February 1, 2007
- DOI: https://doi.org/10.3803/jkes.2007.22.1.8
- 1,631 View
- 22 Download

- A Case of Pituitary Macroadenoma Accompanied with CRH Deficiency.
- Yoo Jung Nahm, Jin Soo Kim, Keun Jong Cho, Uk Hyun Kil, Sung Yong Woo, Sung Rae Kim, Soon Jib Yoo, Sung Koo Kang, Ho Young Son
- J Korean Endocr Soc. 2006;21(2):153-157. Published online April 1, 2006
- DOI: https://doi.org/10.3803/jkes.2006.21.2.153
- 1,673 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - Pituitary tumor can be accompanied with various pituitary hormone abnormalities. Pituitary tumors can be divided into functioning or nonfunctioning tumors. A functioning pituitary tumor, via the oversecretion of pituitary hormones, causes diverse clinical features. A nonfunctioning pituitary tumor can be accompanied with pituitary dysfunction and this may be due to compression or destruction of normal pituitary tissue, suppression of the pituitary portal system or direct damage to the hypothalamus. Corticotropin-releasing hormone (CRH) deficiency, which is caused by defects in the synthesis or release of CRH, is a cause of secondary adrenocortical insufficiency. The clinical presentations are hypoglycemia, weight loss, anemia, weakness, nausea, vomiting and hyponatremia. Acquired CRH deficiency has also been suggested to occur based on a lack of adrenocorticotropic hormone (ACTH) response to insulin-induced hypoglycemia, but there is a normal ACTH response to exogenous CRH. We experienced a case of a woman with pituitary macroadenoma accompanied with CRH deficiency. We report here on this case with the review of the literature.

- A Case of the Milk-alkali Syndrome During Management of Idiopathic Hypoparathyroidism.
- Yong Wan Park, Sung Rae Kim, Jung Min Lee, Seong Hun Kim, Sang Woo Han, Soon Jib Yoo, Kun Ho Yoon, Moo Il Kang, Bong Yun Cha, Kwang Woo Lee, Ho Young Son, Sung Koo Kang
- J Korean Endocr Soc. 2004;19(4):439-445. Published online August 1, 2004
- 1,111 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - Idiopathic hypoparathyroidism is a relatively rare disease characterized by hypocalcemia and hyperphosphatemia: this is due to a deficiency or a sereretory disorder of the parathyroid hormone without any prior operation nor underlying medical disoder. Calcium carbonate and vitamin D substitution are generally considered as the mainstay of therapy, but these treatments can cause hypercalcemia and hypercalciuria. Persistent ingestion of large amount of calcium carbonate can cause milk-alkali syndrome that is characterized by hypercalcemia, metabolic alkalosis and renal failure. Once a patient is diagnosed with milk-alkali syndrome, withdrawal of calcium carbonate and vitamin D is essential and treatment with saline diuresis and furosemide is the usually effective. In treatmenf of hypoparathyroidism with calcium carbonate and vitamin D substitution, evaluation of serum calcium and urinary calcium excretion is essential to avoid hypercalcemia and ypercalciuria. We concluded that during treatment with calcium carbonate and vitamin D substitution for patients with idiopathic hypoparathyroidism, they should have carefully laboratory monitoring, and they should be made aware of the circumstances influencing calcium metabolism


 KES
KES

 First
First Prev
Prev



